Diagnosed with Non-Melanoma Skin Cancer? We Have a Treatment for You!
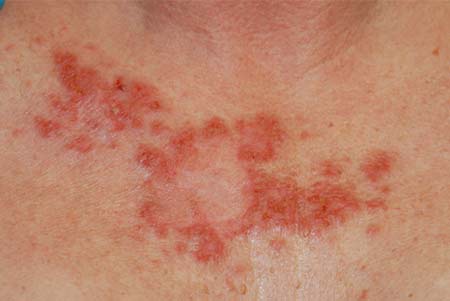
Non-Melanoma Skin Cancer
Non-Melanoma Cancer Treatment
It is important you get treatment today for your Non-melanoma Skin Cancer. Miami Center for Dermatology just got the latest non-invasive radiation treatment for non-melanoma skin cancer. We have placed the article below from the American Cancer Society for you to educate yourself on how important it is to get early treatment.
A study published in the Journal of the National Cancer Institute found that people with a history of basal or squamous cell skin cancer (also known as non-melanoma skin cancer) were at an increased risk of developing other cancers later on. The research suggests genetic factors may put some people at a higher cancer risk than others.
“There appears to be a heightened overall cancer risk associated with Non-Melanoma Skin Cancer, and the evidence seems to indicate that genetic factors are involved,” said lead researcher Anthony J. Alberg, Ph.D., from the Medical University of South Carolina.
Patients with a history of basal or squamous cell skin cancer shouldn’t panic, however.
“This study indicates that a personal history of Non-Melanoma Skin Cancer may be a more important part of a person’s health history than previously thought,” said Alberg. “But the research is preliminary.”
Alberg, along with colleagues from the National Cancer Institute, Johns Hopkins University, and the Medical University of South Carolina, used data from the CLUE (Give Us a Clue to Cancer and Heart Disease) II cohort study to compare risk in 769 non-melanoma cancer survivors and 18,405 individuals who never had the disease.
What the Study Found
The researchers tracked the two groups over a period of 16 years – from May 1989 to December 2005 — and found that those patients with a history of skin cancer had about twice the risk of developing another type of cancer, even after adjusting for other risk factors, including age, sex, body mass index, education, skin type, sunburn history, and smoking history.
“We found that even after adjusting for all factors, there was a doubling of risk for subsequent cancers among Non-Melanoma Skin Cancer patients,” said Alberg.
The most frequently diagnosed cancers were also the most common in the United States: lung, colorectal, breast, and prostate cancer. Unsurprisingly, the increased risk was highest for melanoma, cancer that is also linked to sun exposure, but the increased risk for other cancers remained statistically significant even when the researchers removed melanoma from the group.
Patients who were diagnosed with Non-Melanoma Skin Cancer at an earlier age — in the 25-44 year age group – were more likely to be diagnosed with subsequent cancer later on – a pattern that researchers think points to a genetic susceptibility in some people to develop cancer.
Alberg thinks the answer to this lies in the DNA. He plans to study DNA repair mechanisms as well as inflammatory and immune responses in this population to look for possible links.
Controlling Your Risk
In the meantime, you can minimize your cancer risk by avoiding smoking, limiting your alcohol intake, protecting yourself from the sun, maintaining a healthy weight, getting regular exercise, and adding more fruits and veggies to your diet. To find out more about how you can reduce your risk, see Cancer Prevention and Early Detection and Nutrition and Physical Activity for Cancer Prevention.
Cancer screening tests are also important because cancers that are found early are easier to treat. People who have had any type of skin cancer should take special care to check for new skin cancers, but screening recommendations for other types of cancer are the same as those for the general population. See the American Cancer Society’s Guidelines for the Early Detection of Cancer to learn more about screening exams for different types of cancer.
Citation: “Nonmelanoma Skin Cancer and Risk for Subsequent Malignancy.” Published in the September 3, 2008 issue of the Journal of the National Cancer Institute. Corresponding author: Anthony J. Alberg, Department of Biostatistics, Bioinformatics, and Epidemiology, Hollings Cancer Center. The University of South Carolina.
Original Article by: http://www.cancer.org/cancer/news/news/non-melanoma-skin-cancer-linked-to-risk-of-other-cancers